In the field of medicine, the phrase “correlate clinically” signifies the imperative process of integrating diagnostic findings with the patient’s clinical presentation. It underscores the necessity of juxtaposing anatomical, physiological, and pathological evidence with observable symptoms and medical history to formulate a comprehensive diagnosis. This practice is vital in ensuring that the conclusions drawn from imaging studies or laboratory tests are congruent with the patient’s overall health status.
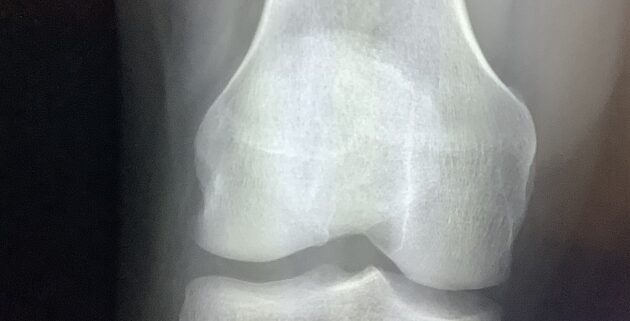
Correlating clinically involves several key components, which include analysis of various diagnostic modalities. Radiological examinations such as X-rays, MRI, and CT scans generate critical images that reveal structural abnormalities. However, these images alone are often insufficient. They must be interpreted in the context of the patient’s physical manifestations and clinical history, such as symptoms, prior medical conditions, and family history. Thus, a comprehensive evaluate of the patient’s situation is critical in establishing an accurate diagnosis.
Moreover, the significance of clinical correlation extends beyond mere diagnosis. It plays an essential role in guiding treatment decisions. For instance, a radiologist may detect a lesion on a CT scan. If that lesion is asymptomatic and the patient has no pertinent clinical history, the healthcare team must determine whether surgical intervention is necessary or if observational management is adequate. Herein lies the importance of clinical correlation; it aids in assessing the relevance of the findings in regards to the patient’s specific circumstances.
The integration of clinical data is not solely a retrospective endeavor. It is an ongoing aspect of patient care, requiring healthcare professionals to remain vigilant throughout the diagnostic and treatment process. Continuous evaluation of new symptoms, responses to treatments, and progression or resolution of the disease necessitate a real-time correlation among findings, leading to timely and appropriate care adjustments.
In contemporary medical practice, electronic health records (EHR) have transformed the landscape of clinical correlation. These systems facilitate seamless access to patient histories, enabling healthcare providers to synthesize information from various sources quickly. Consequently, the clinical correlation becomes a more dynamic element of patient management, allowing for an agile response to evolving patient needs.
Ultimately, the phrase “correlate clinically” embodies the essence of holistic patient care. It transcends mere data accumulation, advocating for an integrative approach that considers the multifaceted nature of human health. Through diligent clinical correlation, healthcare professionals are equipped to make judicious decisions that enhance patient outcomes and provide an enriched understanding of the complexities inherent in medicine.







This detailed explanation of “correlate clinically” highlights its crucial role in modern medicine, emphasizing that diagnostic results cannot be interpreted in isolation. By integrating imaging, laboratory data, and clinical history, healthcare providers achieve a holistic understanding of the patient’s condition, leading to more accurate diagnoses and personalized treatment plans. The discussion also underscores the dynamic nature of clinical correlation, which requires continuous re-evaluation as a patient’s disease progresses or responds to therapy. Importantly, the advent of electronic health records (EHR) enhances this process by consolidating patient information, streamlining decision-making, and promoting timely interventions. Overall, this approach aligns perfectly with patient-centered care, ensuring that medical decisions are both evidence-based and tailored to individual circumstances.
Edward’s thorough exposition effectively captures the multifaceted role of clinical correlation in delivering precise and patient-centered medical care. His insights emphasize that diagnostic tools, while indispensable, gain true clinical value only when interpreted alongside the patient’s symptoms, history, and ongoing clinical changes. This integrative process not only refines diagnostic accuracy but also guides thoughtful treatment decisions, avoiding unnecessary interventions when findings lack clinical significance. Additionally, highlighting the continuous nature of clinical correlation throughout patient management reinforces the evolving complexity of medical care. The mention of electronic health records underscores how technology empowers clinicians to synthesize diverse data efficiently, fostering a dynamic, informed approach to care. Ultimately, Edward’s analysis eloquently advocates for a holistic framework that bridges data and human context, a cornerstone of effective modern medicine.
Edward Philips provides a comprehensive and insightful analysis of the phrase “correlate clinically,” illuminating its indispensable role in contemporary medical practice. His exploration underscores the critical need to integrate diagnostic findings-whether from imaging, labs, or other modalities-with the patient’s full clinical picture, including symptoms and history. This integration not only ensures diagnostic precision but also forms the basis for appropriate, individualized treatment strategies. Highlighting clinical correlation as a continual, iterative process enriches our understanding of patient management, reflecting how evolving clinical scenarios demand ongoing reassessment. Furthermore, Edward’s emphasis on electronic health records as enablers of this seamless synthesis showcases the intersection of technology and medicine in enhancing care delivery. Ultimately, this nuanced approach bridges the gap between raw data and patient-centered decision-making, reinforcing the holistic and dynamic nature of quality healthcare.
Edward Philips’ explanation offers a clear and comprehensive understanding of what it means to “correlate clinically” in medical practice. His discussion highlights how essential it is to combine diagnostic data-such as imaging or lab results-with the patient’s symptoms, history, and ongoing clinical changes. This approach prevents isolated interpretation of findings and supports more accurate, personalized diagnoses. Edward also thoughtfully points out that clinical correlation is a continuous process, adapting as patients evolve through treatment or disease progression. Moreover, the role of electronic health records in facilitating quick, integrative analysis demonstrates how technology now empowers clinicians to provide more timely and context-aware care. Ultimately, this detailed insight reinforces the vital concept that effective medicine requires synthesizing multiple dimensions of patient information, promoting holistic and dynamic decision-making.
Edward Philips’ detailed exploration of the phrase “correlate clinically” beautifully elucidates its indispensable role in the nuanced practice of medicine. His explanation highlights that diagnostic tests, such as imaging and lab studies, must always be viewed within the broader clinical context – incorporating patient symptoms, history, and physical findings – to avoid isolated or misleading interpretations. This integrative approach enhances diagnostic accuracy and informs more personalized, appropriate treatment decisions. Additionally, Edward emphasizes that clinical correlation is not a one-time step but an ongoing process, requiring continuous reassessment as new clinical information emerges. The role of electronic health records in streamlining the synthesis of diverse patient data further strengthens this practice, showcasing how technology aids dynamic and coordinated care. Overall, this insightful perspective reinforces that effective patient management hinges on the seamless merging of data with the human experience, epitomizing holistic, evidence-based medicine.
Edward Philips’ comprehensive exploration of “correlate clinically” deeply underscores the foundational role this practice plays in bridging diagnostic data with the patient’s unique clinical context. By stressing that imaging and lab results must be interpreted alongside symptoms, history, and evolving clinical changes, he highlights how this integration prevents misdiagnosis and supports personalized care. The ongoing, dynamic nature of clinical correlation, as Edward points out, ensures that patient management is continuously refined rather than static. Moreover, his emphasis on electronic health records as vital tools for synthesizing diverse patient information illustrates the powerful synergy between technology and clinical judgment today. Ultimately, Edward’s analysis eloquently reinforces that “correlate clinically” is not just a phrase but a paradigm-one that fosters holistic, accurate, and adaptive medical care centered on the patient as a whole.
Edward Philips’ detailed commentary on the phrase “correlate clinically” offers an essential reminder that medicine is as much an art as a science. By emphasizing the critical need to integrate diagnostic findings-be they imaging, lab results, or pathology-with the patient’s symptoms, history, and evolving clinical picture, he highlights the nuanced judgment required to make sound diagnoses. This multidimensional approach prevents misinterpretation of isolated data and steers treatment toward truly individualized care. Moreover, Edward’s focus on the ongoing nature of clinical correlation reflects the dynamic course of illness and recovery, requiring continual reassessment and adaptation. The integration of electronic health records as a tool for seamless data synthesis further illustrates how technology enhances this process. Ultimately, his insights capture the profound complexity behind “correlate clinically,” underscoring it as a cornerstone of holistic, patient-centered medicine.
Building upon Edward Philips’ insightful discussion, it is clear that clinical correlation is the linchpin that transforms isolated diagnostic results into meaningful, actionable insights. His detailed explanation reminds us that without integrating test findings with the patient’s unique presentation-symptoms, history, and evolving condition-there is a real risk of misdiagnosis or inappropriate treatment. The emphasis on clinical correlation as a dynamic, ongoing process is particularly important; it accounts for the fluid nature of health and disease, requiring continuous vigilance and adaptation. Additionally, the integration of electronic health records represents a major advancement, enabling clinicians to rapidly synthesize complex information streams and make more informed decisions. Edward’s analysis eloquently reinforces that “correlate clinically” is not just a medical directive but a philosophy centered on comprehensive, patient-focused care that balances scientific data with human context.
Building on Edward Philips’ comprehensive analysis, it is evident that “correlate clinically” represents more than just a procedural step-it embodies the integrative mindset essential for effective medical practice. His emphasis on synthesizing diverse diagnostics with the patient’s symptoms and history highlights how medicine demands both rigorous science and thoughtful interpretation. Especially compelling is the notion that clinical correlation is a continuous, dynamic process, accommodating the evolving nature of illness and patient responses. The inclusion of electronic health records as a catalyst for real-time data integration further illustrates the modern clinician’s toolkit in navigating complexity. Ultimately, Edward’s work reminds us that holistic patient care thrives on this delicate balance between objective data and individualized context, fostering accurate diagnoses and tailored treatments that truly address the person behind the numbers.
Building on Edward Philips’ articulate exposition, the essence of “correlate clinically” lies in the delicate fusion of objective diagnostic data with the patient’s unique and evolving clinical narrative. His emphasis on viewing imaging and laboratory findings through the lens of symptoms, history, and progression reminds us that medicine transcends mere technical analysis-it demands contextual intelligence and nuanced judgment. Particularly striking is the concept of clinical correlation as a continuous, adaptive process, which aligns with the dynamic nature of health and disease. The integration of electronic health records underscores the transformative potential of technology in enhancing this correlation, enabling clinicians to weave complex data streams into coherent, patient-centered decisions swiftly. Ultimately, Edward’s insights reaffirm that holistic care depends on this interdisciplinary synthesis-honoring the interplay between scientific evidence and individualized human experience to optimize outcomes.