Healthcare providers dedicate their lives to safeguarding the well-being of others. Inherent to this commitment is the responsibility to protect themselves, thereby minimizing the risk of transmitting infectious diseases to vulnerable patients. Vaccination stands as the cornerstone of this protection, a shield not only for the individual practitioner but also for the entire healthcare ecosystem. This detailed guide outlines the essential vaccines that every healthcare provider should consider, ensuring they are adequately protected against preventable diseases.
Influenza Vaccine: The Annual Imperative
Influenza, commonly known as the flu, poses a significant threat, particularly during the winter months. Healthcare settings are prime breeding grounds for viral transmission. An annual influenza vaccine is not merely a recommendation; it’s a professional obligation. The antigenic drift of the influenza virus necessitates yearly reformulation of the vaccine. Healthcare providers should receive their flu shot early in the season, ideally by the end of October, to achieve optimal immunity before the peak of influenza activity. Different formulations are available, including quadrivalent vaccines offering protection against four strains of influenza, and high-dose vaccines tailored for older adults.
Measles, Mumps, and Rubella (MMR) Vaccine: Establishing Robust Immunity
Measles, mumps, and rubella are highly contagious viral diseases. While childhood vaccination has significantly reduced their incidence, outbreaks can still occur. Healthcare providers should have documented evidence of immunity to these diseases, either through vaccination or serologic testing confirming the presence of antibodies. If immunity is lacking, two doses of the MMR vaccine are recommended, administered at least 28 days apart. Prioritizing this is crucial, especially for those working with pediatric populations or in areas with known outbreaks.
Varicella (Chickenpox) Vaccine: Preventing a Resurgence
Varicella-zoster virus causes both chickenpox and shingles. Healthcare providers who lack a history of chickenpox or laboratory evidence of immunity should receive the varicella vaccine. Two doses are required, spaced four to eight weeks apart. This vaccine prevents the primary varicella infection (chickenpox) and reduces the risk of developing shingles later in life, a particularly debilitating condition. Vaccination is vital for healthcare personnel in contact with immunocompromised patients, who are at high risk of severe varicella complications.
Tetanus, Diphtheria, and Pertussis (Tdap) Vaccine: Ensuring Waning Immunity is Bolstered
Tetanus, diphtheria, and pertussis are bacterial infections that can have serious consequences. Healthcare providers should receive a Tdap booster once as adults, regardless of their prior Td vaccination history. This booster is especially important for protection against pertussis, commonly known as whooping cough, which can be severe and even fatal in infants. Subsequent boosters with Td (tetanus and diphtheria) are recommended every 10 years to maintain adequate protection.
Hepatitis B Vaccine: A Shield Against Occupational Exposure
Hepatitis B is a viral infection that can cause chronic liver disease and liver cancer. Healthcare providers, particularly those involved in direct patient care or handling blood and body fluids, are at increased risk of occupational exposure. The hepatitis B vaccine is administered as a three-dose series. Post-vaccination antibody testing is recommended to confirm seroconversion, indicating successful immunity. If seroconversion does not occur after the initial series, a second series of three doses may be necessary.
COVID-19 Vaccine: A Contemporary Mandate
The COVID-19 pandemic has underscored the importance of vaccination as a primary defense against infectious diseases. Vaccination against SARS-CoV-2, the virus that causes COVID-19, is a paramount consideration for healthcare providers. The specific vaccine recommendations, including the primary series and booster doses, may evolve based on emerging data and variant strains. It’s imperative for healthcare personnel to stay informed about the latest guidelines from public health authorities like the CDC and adhere to institutional policies regarding COVID-19 vaccination.
Meningococcal Vaccine: Protection Against Invasive Disease
Meningococcal disease is a serious bacterial infection that can cause meningitis and septicemia. While not routinely recommended for all healthcare providers, vaccination may be warranted for those working in specific settings, such as student health centers or facilities experiencing outbreaks. Two types of meningococcal vaccines are available: conjugate vaccines (MenACWY) and serogroup B vaccines (MenB). The specific vaccine recommendations depend on the individual’s age, risk factors, and the circulating serogroups in their region.
Special Considerations and Situational Vaccines
Certain healthcare providers may require additional vaccines based on their specific roles and potential exposures. For example, those working with laboratory animals may need rabies and Q fever vaccines. Travel to endemic areas may necessitate vaccines against diseases such as yellow fever, typhoid fever, and Japanese encephalitis. A thorough risk assessment, conducted in consultation with occupational health professionals, can identify these individualized vaccination needs. Pregnant healthcare providers require special consideration regarding vaccine safety and efficacy during gestation.
Maintaining Accurate Vaccination Records and Advocating for Vaccination
Healthcare providers should maintain accurate and up-to-date vaccination records. These records should include the dates of vaccination, the vaccine manufacturer and lot number, and any adverse reactions experienced. Sharing vaccination records with employers and participating in immunization registries helps track vaccination rates and identify gaps in coverage. Furthermore, healthcare providers should actively advocate for vaccination among their patients and colleagues, dispelling misinformation and promoting the benefits of immunization. Promoting vaccination contributes to herd immunity, protecting vulnerable populations who cannot be vaccinated due to medical contraindications.
In conclusion, vaccination is an ethical and professional imperative for all healthcare providers. By prioritizing their own health and protecting themselves from preventable diseases, healthcare personnel can safeguard the well-being of their patients and contribute to a healthier community. Remaining informed about the latest vaccine recommendations and engaging in open communication with healthcare professionals ensures optimal protection against infectious diseases.

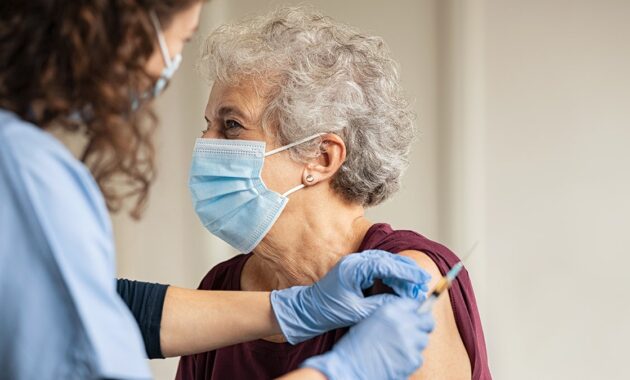






This comprehensive guide emphasizes the critical role vaccination plays in protecting healthcare providers and the patients they serve. By detailing essential vaccines-from the annual influenza shot to specialized vaccines like meningococcal and occupationally indicated ones-the article underscores vaccination as both a personal and professional responsibility. It highlights how staying up-to-date with vaccines not only reduces the risk of disease transmission within healthcare settings but also helps maintain herd immunity in the broader community. The inclusion of specific recommendations, such as timing for flu vaccines and the need for boosters, offers practical guidance. Furthermore, addressing situational vaccines and the importance of accurate record-keeping reflects a thorough approach to occupational health. Ultimately, this resource serves as a vital reminder that protecting healthcare workers through vaccination is foundational to ensuring patient safety and public health.
Amanda Graves’ detailed exploration of essential vaccinations for healthcare providers underscores an often underappreciated aspect of patient safety: the health of the caregiver. By systematically outlining vaccines like influenza, MMR, varicella, Tdap, and hepatitis B, among others, this guide not only clarifies the direct protective benefits to healthcare workers but also highlights their role in preventing disease transmission to vulnerable patient populations. The emphasis on up-to-date immunization, coupled with situational considerations and accurate record-keeping, reflects a pragmatic and holistic approach to occupational health. Importantly, Amanda’s inclusion of the evolving COVID-19 recommendations and special scenarios, such as travel or pregnancy, illustrates the dynamic nature of vaccination needs in healthcare. This comprehensive approach empowers healthcare professionals to advocate for vaccination confidently, promoting a safer clinical environment and enhancing community-wide public health.
Amanda Graves’ thorough breakdown eloquently captures the multifaceted importance of vaccination in healthcare settings. Beyond personal protection, vaccines serve as a critical barrier against the spread of infectious diseases to vulnerable patients, highlighting healthcare providers’ dual role as both caregivers and public health guardians. The guide’s detailed review-from annual influenza immunization to specialized vaccines based on occupational risks-emphasizes that vaccine strategies must be dynamic and tailored. Attention to record-keeping and advocacy further enhances the healthcare workforce’s ability to maintain community-wide immunity. Particularly timely is the discussion of COVID-19 vaccination, reflecting evolving challenges. This comprehensive framework not only supports individual health but also strengthens institutional resilience and patient trust, reinforcing vaccination as a core ethical and professional mandate in healthcare.
Amanda Graves’ detailed exposition on healthcare provider vaccinations is a vital reminder of the interconnectedness between individual immunity and community health within clinical settings. Her comprehensive overview not only delineates the essential vaccines but also contextualizes their importance in reducing healthcare-associated infections and safeguarding vulnerable patient populations. The emphasis on annual updates, such as the influenza vaccine, and tailored immunizations based on exposure risks illustrates the nuanced approach necessary for effective occupational health. Additionally, Amanda’s focus on meticulous record-keeping and advocacy underscores the role of healthcare workers as both recipients and promoters of immunization, fostering a culture of safety and trust. This guide adeptly navigates contemporary challenges, including COVID-19, making it an indispensable resource for frontline professionals committed to ethical and evidence-based practice.
Amanda Graves delivers an indispensable guide that expertly highlights the vital role of vaccination in protecting healthcare providers and the communities they serve. Her detailed breakdown of routine vaccines, such as influenza, MMR, varicella, Tdap, and hepatitis B, underscores the importance of proactive immunity in preventing disease transmission within healthcare settings. The article thoughtfully addresses special circumstances like occupational risks, travel-related immunizations, pregnancy, and the evolving COVID-19 recommendations, reflecting the dynamic nature of vaccine needs. Additionally, Amanda’s emphasis on maintaining accurate records and advocating for immunization fosters a culture of responsibility and trust, essential for sustaining herd immunity. This comprehensive overview not only empowers healthcare workers to safeguard their own health but also reinforces their ethical duty to protect vulnerable patients, making it a crucial resource for maintaining safe and resilient healthcare environments.