The ways in which countries remunerate healthcare providers is a subject of enduring fascination. It touches upon fundamental questions about societal values, economic models, and the very nature of health as a human right. The variation in approaches reflects diverse philosophical underpinnings regarding the role of government, individual responsibility, and the optimal allocation of scarce resources. It’s a complex tapestry woven from political ideologies, historical precedent, and pragmatic considerations. Let’s delve into this intricate landscape.
I. Fee-for-Service (FFS): The Volume-Driven Model
One prevalent paradigm is the Fee-for-Service (FFS) system. Under FFS, healthcare providers are compensated for each individual service rendered. This might encompass a consultation, a diagnostic test, a surgical procedure, or the administration of a medication. The inherent allure of FFS lies in its apparent simplicity and its potential to incentivize productivity. Providers are directly rewarded for the volume of services they deliver. However, this very incentive structure can be a double-edged sword. It can contribute to overutilization and the performance of medically unnecessary procedures, driving up healthcare costs without necessarily improving patient outcomes. Furthermore, FFS models can incentivize quantity over quality, potentially leading to fragmented care and a lack of coordination between providers. The United States, in particular, relies heavily on FFS models, though there are ongoing efforts to transition towards value-based care.
II. Capitation: A Population-Based Approach
Capitation represents a fundamentally different approach to provider remuneration. Instead of paying for each service, providers receive a fixed payment per patient enrolled in their practice or health plan, regardless of the number of services they provide. This approach is often used in primary care settings, encouraging providers to manage the overall health of their patient panel. The primary advantage of capitation is that it incentivizes preventive care and disease management. By receiving a fixed payment, providers are motivated to keep their patients healthy and avoid costly hospitalizations. However, capitation also carries the risk of under-provision of care. Providers may be tempted to limit services to stay within their budget, potentially compromising patient health. Therefore, robust quality monitoring and performance measurement are crucial to ensuring that capitation arrangements deliver high-quality care.
III. Salary: The Public Sector Standard
In many countries with publicly funded healthcare systems, providers are salaried employees of the government or a public institution. This is particularly common in countries with national health services, such as the United Kingdom and Canada. Salaried physicians receive a fixed salary regardless of the number of patients they see or the services they provide. This model offers stability and predictability for both providers and the healthcare system. It also aligns provider incentives with the overall goals of the healthcare system, such as promoting access and equity. However, salary models can sometimes be criticized for stifling innovation and reducing provider motivation. Without direct financial incentives linked to performance, providers may be less motivated to go the extra mile for their patients. Effective performance management systems and opportunities for professional development are essential to maintaining high levels of provider engagement in salaried systems.
IV. Global Budgeting: Managing Healthcare Expenditures at the Macro Level
Global budgeting involves allocating a fixed sum of money to a hospital, region, or healthcare system to cover all of its operating expenses for a given period. This approach provides a strong incentive for cost control and resource management. Hospitals and healthcare systems must operate within their allocated budget, encouraging them to find efficiencies and reduce waste. Global budgeting can also promote better coordination of care, as providers are incentivized to work together to manage resources effectively. However, global budgeting can also lead to rationing of care, particularly if budgets are insufficient to meet the needs of the population. Waiting lists may lengthen, and access to certain services may be restricted. Careful planning and monitoring are essential to ensure that global budgeting does not compromise patient care.
V. Blended Payment Models: Seeking the Best of Both Worlds
Recognizing the limitations of any single payment model, many countries are experimenting with blended payment models that combine elements of FFS, capitation, and salary. For example, a primary care physician might receive a capitation payment for each patient enrolled in their practice, plus a fee for specific services, such as immunizations or chronic disease management. This approach seeks to balance the incentives for volume and value, encouraging providers to provide both preventive care and high-quality treatment. Blended payment models can be complex to design and implement, but they hold the promise of improving both the efficiency and the quality of healthcare.
VI. The Rise of Value-Based Care: Paying for Outcomes, Not Just Services
A growing trend in healthcare payment is the shift towards value-based care. Value-based care models focus on paying providers for the quality and outcomes of their care, rather than simply the volume of services they provide. This can involve a variety of approaches, such as pay-for-performance, bundled payments, and accountable care organizations (ACOs). Pay-for-performance programs reward providers for meeting specific quality targets, such as reducing hospital readmission rates or improving patient satisfaction. Bundled payments provide a single payment for all of the services associated with a particular episode of care, such as a hip replacement or a pregnancy. ACOs are groups of providers who work together to coordinate care for a defined population of patients, sharing in the savings generated by improving quality and reducing costs. Value-based care models hold the promise of transforming healthcare by aligning provider incentives with patient needs and promoting a focus on outcomes.
VII. The Technological Transformation: How Informatics Influences Reimbursement
The burgeoning field of health informatics profoundly impacts how providers are reimbursed. Sophisticated data analytics can track patient outcomes, identify cost drivers, and measure the effectiveness of different interventions. This data can be used to refine payment models and ensure that resources are allocated efficiently. Furthermore, electronic health records (EHRs) facilitate the collection and sharing of data, making it easier to monitor quality and performance. Telehealth, enabled by digital technologies, is also transforming healthcare delivery and creating new opportunities for reimbursement, particularly in underserved areas. The judicious application of technology is becoming an indispensable tool in the quest for more efficient and effective healthcare payment systems.
Ultimately, the optimal approach to paying healthcare providers is a matter of ongoing debate and experimentation. There is no one-size-fits-all solution. The best approach will depend on the specific context, including the country’s healthcare system, its cultural values, and its economic resources. As nations grapple with the challenges of rising healthcare costs and aging populations, the search for innovative and sustainable payment models will continue. The goal remains constant: to ensure that patients receive high-quality, affordable care that meets their needs and improves their health outcomes. The delicate balance between incentivizing efficiency and ensuring equitable access remains the paramount consideration.

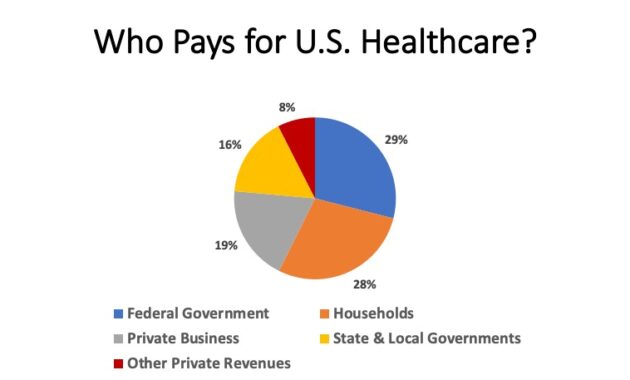





This comprehensive exploration into healthcare provider remuneration highlights the intricate balance between incentivizing quality care and managing costs within diverse health systems. By dissecting models such as Fee-for-Service, Capitation, Salary, Global Budgeting, and blended approaches, it becomes clear that no single system perfectly addresses the multifaceted challenges healthcare faces today. The shift towards value-based care underscores a crucial transformation-prioritizing patient outcomes over sheer service volume to improve efficiency and equity. Additionally, the integration of health informatics and telehealth exemplifies how technology can refine reimbursement strategies and foster innovation. Ultimately, this nuanced overview reminds us that sustainable healthcare financing must align with societal values, address economic realities, and continuously adapt to evolving patient needs, ensuring access and quality remain central goals across different contexts.
Amanda Graves’ thorough analysis eloquently captures the complexity and diversity of healthcare provider payment systems worldwide. It skillfully balances the practical advantages and pitfalls of each model-from the volume incentives inherent in Fee-for-Service to the preventive focus encouraged by Capitation, and the stability provided by salaried positions. The discussion of global budgeting and blended models also highlights the ongoing quest to reconcile cost containment with high-quality, accessible care. Notably, the emphasis on value-based care signals a paradigm shift towards outcome-oriented reimbursement, aligning financial incentives with patient well-being rather than service quantity. The integration of health informatics and telehealth further illustrates how technology is reshaping payment frameworks by enhancing data-driven decision-making and expanding care access. This comprehensive exploration underscores that no universal solution exists; instead, adaptive, context-specific approaches remain essential for sustainable healthcare financing that serves both providers and patients effectively.
Amanda Graves provides a nuanced and comprehensive overview that highlights just how multifaceted and context-dependent healthcare provider payment systems are. The synthesis of various remuneration models-from Fee-for-Service to Capitation, Salary, and Global Budgeting-aptly reveals that each embodies distinct incentives and risks. Particularly striking is the discussion of blended models and value-based care, which illustrate an evolution towards payment structures that better align provider motivations with patient outcomes and system sustainability. The integration of health informatics and telehealth further underscores technology’s transformative potential in enhancing transparency, efficiency, and accessibility. Graves reminds us that while no single payment model is flawless, ongoing innovation and adaptation, grounded in cultural and economic realities, are critical to achieving equitable, high-quality care amid ever-growing healthcare demands. This piece encourages continued dialogue and experimentation in the pursuit of a balanced and effective remuneration system.
Amanda Graves’ insightful analysis articulates the complexities inherent in healthcare provider payment systems, effectively illustrating how each model carries distinct incentives that shape provider behavior and health outcomes. The coverage of traditional models like Fee-for-Service and Capitation versus emerging frameworks such as value-based care reveals a landscape in transition-a dynamic interplay between rewarding volume and promoting quality. Particularly compelling is the discussion on blended payment strategies, reflecting a pragmatic recognition that hybrid approaches may best reconcile efficiency, equity, and quality goals. The role of health informatics and telehealth further enriches this discourse, highlighting technology’s growing power to make reimbursement more data-driven and patient-centered. Graves rightly underscores that no universal payment model fits all contexts; ongoing innovation, mindful of local cultural, economic, and systemic factors, remains essential in crafting sustainable healthcare financing that benefits both patients and providers alike.
Amanda Graves offers a masterful synthesis of healthcare provider remuneration, illuminating the intricate interplay between economic incentives, patient outcomes, and system sustainability. By dissecting classic models like Fee-for-Service, Capitation, and Salary alongside emerging approaches such as value-based care and blended payment systems, the analysis captures the evolving efforts to reconcile volume-driven incentives with quality and prevention. The inclusion of global budgeting highlights the macro-level fiscal constraints shaping care delivery, while the focus on health informatics and telehealth underscores the transformative role of technology in driving data-informed reimbursement strategies. As the commentary underscores, the “one-size-fits-all” solution remains elusive; thoughtful adaptation to local cultural, economic, and institutional contexts is imperative. Graves’ comprehensive perspective invites ongoing innovation and dialogue, reinforcing the imperative to craft payment systems that equitably balance efficiency, access, and patient-centered care in an era of complex healthcare challenges.