The healthcare ecosystem, a complex and multifaceted arena, functions through the intricate interplay of various entities. Among the most pivotal are payers and providers. Understanding their distinct roles and collaborative dynamics is crucial for navigating the labyrinthine world of healthcare. This article aims to elucidate the functions, variations, and interconnectedness of these two essential components of the system.
Defining the Players: Payers and Providers
At their core, payers are entities that finance healthcare services. They bear the financial risk associated with providing medical care to a defined population. Conversely, providers are the individuals or organizations that deliver healthcare services directly to patients. This can encompass a wide array of professionals and institutions, all dedicated to maintaining and improving the health of individuals.
The Spectrum of Payers: A Detailed Examination
The payer landscape is diverse, encompassing both public and private entities. Each type of payer operates under a different framework, influencing coverage options, reimbursement models, and patient access to care. Let’s delve into the key categories:
Public Payers: Government-Sponsored Healthcare
- Medicare: A federal health insurance program primarily for individuals aged 65 and older, as well as certain younger people with disabilities or chronic conditions. Medicare encompasses various parts, including Part A (hospital insurance), Part B (medical insurance), Part C (Medicare Advantage), and Part D (prescription drug coverage). Understanding these distinct components is key to comprehending the scope of Medicare’s benefits.
- Medicaid: A joint federal and state program that provides healthcare coverage to low-income individuals and families. Eligibility criteria and benefits vary significantly from state to state. Medicaid plays a crucial role in ensuring access to care for vulnerable populations.
- Veterans Affairs (VA): The VA provides comprehensive healthcare services to eligible veterans through a network of hospitals and clinics across the country. The VA system is dedicated to addressing the unique healthcare needs of those who have served in the armed forces.
Private Payers: Employer-Sponsored and Individual Insurance
- Employer-Sponsored Insurance: A common form of health insurance where employers offer coverage to their employees and their dependents. These plans often involve a shared cost between the employer and employee, with a variety of coverage options available.
- Individual Health Insurance: Individuals can purchase health insurance directly from private insurance companies. These plans are often obtained through health insurance marketplaces established under the Affordable Care Act (ACA). The ACA has significantly expanded access to individual health insurance, offering subsidies to eligible individuals and families.
- Managed Care Organizations (MCOs): MCOs, such as Health Maintenance Organizations (HMOs) and Preferred Provider Organizations (PPOs), aim to manage healthcare costs and improve quality of care through various strategies, including provider networks, utilization management, and disease management programs.
The Provider Landscape: From Primary Care to Specialized Services
Providers constitute the frontline of healthcare delivery, encompassing a vast array of professionals and institutions. They are the ones who directly interact with patients, diagnosing ailments, administering treatments, and providing ongoing care. Let’s examine the major categories of providers:
Physicians: The Core of Medical Care
- Primary Care Physicians (PCPs): PCPs serve as the initial point of contact for patients, providing comprehensive care for a wide range of medical conditions. They also play a crucial role in coordinating care and referring patients to specialists when necessary.
- Specialists: Physicians who have undergone advanced training in a specific area of medicine, such as cardiology, oncology, or dermatology. Specialists provide expert care for complex medical conditions.
Hospitals and Healthcare Facilities: Centers of Acute Care
- Acute Care Hospitals: These hospitals provide short-term care for patients with acute illnesses or injuries. They offer a wide range of services, including emergency care, surgery, and diagnostic testing.
- Long-Term Care Facilities: These facilities provide care for individuals who require ongoing medical or personal care services, such as nursing homes and assisted living facilities.
Allied Health Professionals: Essential Support for Patient Care
- Nurses: Nurses provide direct patient care, administer medications, and educate patients and families about their health conditions. They play a vital role in ensuring patient safety and well-being.
- Therapists: Physical therapists, occupational therapists, and speech therapists help patients recover from injuries or illnesses and improve their functional abilities.
- Pharmacists: Pharmacists dispense medications, provide drug information, and monitor patients for adverse drug reactions. They are essential members of the healthcare team.
The Interplay: How Payers and Providers Interact
The relationship between payers and providers is fundamental to the functioning of the healthcare system. Payers reimburse providers for the services they render to patients. The terms of these reimbursements are often negotiated through contracts. These contracts dictate the payment rates, billing procedures, and quality metrics that providers must adhere to. The negotiation of these contracts can be complex, involving considerations such as market rates, provider performance, and patient outcomes.
Reimbursement Models: Fee-for-Service vs. Value-Based Care
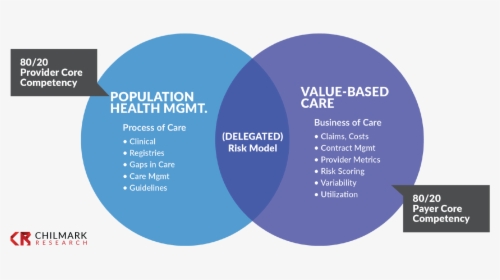
Traditional fee-for-service (FFS) models reimburse providers for each individual service they provide. This model can incentivize providers to order more tests and procedures, potentially leading to higher healthcare costs. Value-based care (VBC) models, on the other hand, aim to incentivize providers to deliver high-quality, cost-effective care. VBC models often involve bundled payments, capitation, and shared savings arrangements. The shift towards VBC is driven by the desire to improve patient outcomes and reduce healthcare spending.
Challenges and Future Directions
The healthcare ecosystem faces numerous challenges, including rising costs, access disparities, and quality concerns. Addressing these challenges requires innovative solutions and collaborative efforts from payers, providers, and policymakers. Embracing technology, promoting preventive care, and fostering patient engagement are essential steps towards building a more sustainable and equitable healthcare system. The future of healthcare hinges on the ability of payers and providers to work together to achieve shared goals of improved health outcomes and affordable access for all.
In conclusion, payers and providers are indispensable components of the healthcare system. Their distinct roles and interdependent relationships are pivotal to ensuring that individuals receive the medical care they need. Comprehending the nuances of their interactions, the diverse types of payers and providers, and the evolving reimbursement models is critical for anyone seeking to navigate the intricacies of the healthcare landscape.







This comprehensive article provides an insightful overview of the healthcare ecosystem by clearly defining the critical roles of payers and providers. It effectively highlights the diversity of payer types, from public programs like Medicare, Medicaid, and VA to private insurance options, emphasizing how each influences access and reimbursement structures. The detailed exploration of providers-from primary care physicians to specialized practitioners and allied health professionals-demonstrates the complexity of care delivery. The discussion on reimbursement models, contrasting fee-for-service with value-based care, underscores the system’s ongoing shift toward incentivizing quality and cost-efficiency. Importantly, the article also addresses current challenges and the need for collaborative innovation among stakeholders. This nuanced understanding of payer-provider dynamics is essential for anyone aiming to grasp the forces shaping healthcare outcomes and affordability today.
Amanda Graves’ article skillfully dissects the intricate relationship between payers and providers within the healthcare ecosystem. By delineating the varied roles and types of payers-from government programs like Medicare, Medicaid, and the VA to diverse private insurance models-the piece sheds light on how financing frameworks directly influence coverage and patient access. Likewise, the thorough overview of providers, ranging from primary care physicians to allied health professionals, highlights the multifaceted nature of care delivery. The examination of reimbursement approaches, contrasting fee-for-service with value-based care, aptly captures the system’s shift toward improving outcomes while controlling costs. Moreover, the article’s emphasis on the necessity for payers and providers to collaborate, innovate, and embrace technology is a timely reflection on the pathway to overcoming systemic challenges in healthcare. Overall, this nuanced portrayal offers readers a foundational understanding of how these core players interact to shape the future of accessible, high-quality healthcare.
Amanda Graves offers a comprehensive and well-structured examination of the healthcare ecosystem by illuminating the distinct yet interconnected roles of payers and providers. Her detailed breakdown of payer types-from public programs like Medicare, Medicaid, and the VA to various private insurance options-underscores the complexity behind coverage decisions and financial risk management. The article’s thorough portrayal of providers, including primary care physicians, specialists, and allied health professionals, paints a clear picture of the multifaceted nature of patient care delivery. The comparison between fee-for-service and value-based reimbursement models is especially salient, capturing a critical transition in healthcare aimed at enhancing quality while containing costs. Furthermore, the discussion on challenges and future directions highlights the imperative for ongoing collaboration, innovation, and technological integration to build a more equitable and effective system. This article is a valuable resource for anyone seeking a deep understanding of how payers and providers jointly shape healthcare today and in the future.