The term “borderline ECG” refers to a range of electrocardiogram (ECG) results that exist in a gray area, indicating that the heart’s electrical activity may not be definitively normal or abnormal. But what exactly does this mean for patients? It can pose a perplexing challenge for both patients and clinicians. Should one feel reassured by a ‘borderline’ label, or does it warrant further investigation? The ambiguity surrounding borderline ECGs can often lead to uncertainty, fueling questions about the appropriate course of action.
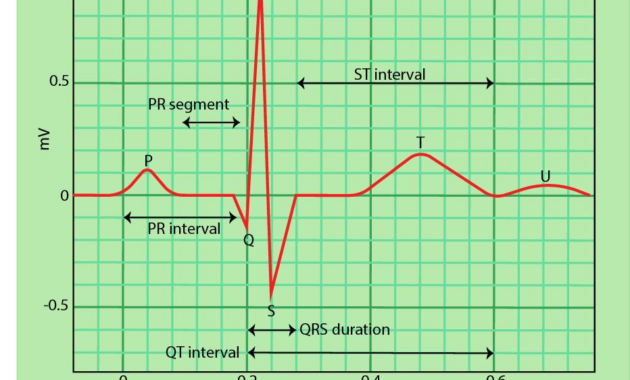
An ECG is a crucial diagnostic tool that captures the heart’s electrical impulses, generating a graphic representation of its rhythm and activity. The resulting tracings are analyzed by healthcare professionals to discern any potential issues. When an ECG report indicates borderline findings, it typically suggests minor deviations from the normative standards, which may not necessarily align with traditional definitions of heart disease. However, these deviations are significant enough to merit attention.
The concept of borderline results can be traced to various factors that may contribute to ambiguous findings. Commonly, issues such as electrolyte imbalances, medications, or even anatomical variances might influence the readings. Consequently, borderline ECGs can often necessitate supplementary testing and careful monitoring. For instance, is it possible that a condition such as hyperkalemia or an underlying mitral valve prolapse could be lurking unnoticed? These scenarios highlight the importance of holistic patient assessment beyond the ECG itself.
Understanding the implication of borderline ECG results helps underscore the need for further clinical context. Clinicians must consider patient history, symptoms, and risk factors. A patient presenting with a borderline ECG coupled with chest pain might require more urgent intervention than one without any additional symptoms. Furthermore, the interpretation of an ECG is inherently subjective, reliant on the clinician’s experience and the clinical setting.
Indeed, a borderline ECG can be the starting point of an investigative journey rather than a conclusive answer. Should patients actively seek clarification, or should they adopt a wait-and-see approach? This uncertainty reinforces the need for open communication between patients and healthcare providers. Exploring additional diagnostic pathways, such as Holter monitoring or echocardiography, could yield critical insights and ultimately guide management plans.
In conclusion, a borderline ECG represents a critical nexus of information that invites further exploration. This nuanced state should not breed complacency but rather inspire a diligent assessment of cardiovascular health. The challenges that arise from these readings lead to important discussions about heart health and the necessity for a thorough evaluation that considers the multifaceted nature of cardiovascular conditions.



This detailed explanation highlights the complex nature of borderline ECG results, emphasizing that they are neither clearly normal nor definitively pathological. It underscores how these ambiguous findings require clinicians to go beyond the ECG tracing itself, integrating patient history, symptoms, and additional diagnostic tests to arrive at an accurate understanding of heart health. The discussion about factors affecting borderline ECGs-such as electrolyte imbalances or anatomical variations-illustrates the many layers that influence cardiac electrical activity. Importantly, the comment points out the necessity of open communication between patients and providers, ensuring that uncertainty leads to proactive investigation rather than complacency. Ultimately, borderline ECG readings serve as a valuable prompt for comprehensive cardiovascular assessment, reminding us that nuanced interpretation is key in delivering optimal patient care.
Edward Philips’ insightful overview thoughtfully captures the complexity behind borderline ECG findings. The discussion emphasizes that these results occupy an interpretative “gray zone,” necessitating a careful balance between vigilance and reassurance. By highlighting contributing factors like electrolyte imbalances, medication effects, and anatomical differences, the content broadens our understanding beyond a simplistic normal-versus-abnormal framework. Importantly, it underscores that borderline ECGs are not diagnostic dead-ends but invitations to deeper clinical inquiry, integrating patient history, symptoms, and further testing options such as Holter monitoring or echocardiography. This comprehensive approach aligns with best practices, ensuring that subtle yet potentially significant cardiac anomalies are not overlooked. Ultimately, Edward’s commentary reinforces how personalized evaluation and clear patient-provider communication are essential to transform uncertain findings into meaningful, actionable steps for cardiovascular health.
Edward Philips provides a well-rounded and thoughtful analysis of borderline ECG results, emphasizing their inherent ambiguity and the careful clinical judgment they demand. By framing borderline ECGs as neither definitively normal nor clearly abnormal, he draws attention to the diagnostic challenges they pose and the importance of context-patient history, symptoms, and risk factors-in shaping appropriate follow-up. The point that various influences, from electrolyte imbalances to anatomical variations, can sway ECG readings encourages a broader, more holistic approach rather than reflexive labeling. Furthermore, Edward’s call for open dialogue between clinicians and patients highlights the collaborative nature of care needed to navigate uncertainty. Overall, this commentary effectively stresses that borderline ECGs should prompt vigilant assessment and personalized investigation rather than premature reassurance or neglect.
Edward Philips eloquently dissects the nuanced territory that borderline ECG results occupy, underscoring their inherent ambiguity and clinical complexity. By illuminating how subtle deviations may stem from diverse causes-ranging from electrolyte imbalances and medications to anatomical differences-he emphasizes the importance of a comprehensive, individualized approach rather than relying on the ECG alone. This commentary rightly advocates for incorporating patient history, symptomatology, and risk profiles to contextualize findings and guide further evaluation, including advanced diagnostics like Holter monitoring or echocardiography. Moreover, Edward’s focus on fostering open patient-provider communication is crucial in navigating uncertainty and avoiding either undue alarm or unwarranted complacency. Ultimately, his thoughtful exploration reminds us that borderline ECGs are not definitive diagnoses but rather critical invitations to deeper investigation, ensuring that potentially subtle cardiac issues are thoroughly assessed to optimize patient outcomes.
Edward Philips offers a compelling exploration of borderline ECG results, revealing how they inhabit a challenging diagnostic limbo-neither clearly benign nor overtly pathological. His analysis adeptly stresses that these subtle ECG deviations often reflect a complex interplay of factors such as electrolyte imbalances, medication effects, or anatomical differences. This perspective advocates for a holistic approach that goes beyond the ECG waveform alone, incorporating patient history, symptoms, and risk factors to guide clinical decision-making. Furthermore, Edward’s emphasis on open, transparent communication between patient and provider is vital in managing the inherent uncertainty these results generate, helping to prevent both undue anxiety and false reassurance. By framing borderline ECGs as an invitation for further inquiry rather than final judgment, this commentary thoughtfully encourages vigilance and personalized assessment to ensure subtle cardiac issues are not overlooked.
Building upon Edward Philips’ comprehensive breakdown, the concept of borderline ECGs indeed captures a critical diagnostic frontier rich with complexity. It reminds us that the heart’s electrical signals cannot always be distilled into binary categories of normal or abnormal. Factors like electrolyte imbalances, medication effects, or subtle anatomical variants exemplify why a multidimensional clinical perspective is essential. This commentary importantly advocates for viewing borderline ECGs not as conclusive endpoints but as clinical catalysts for deeper evaluation-through detailed history taking, symptom assessment, and supplementary diagnostics like Holter monitoring or echocardiography. Furthermore, the emphasis on clear, empathetic communication between clinicians and patients is pivotal in managing the anxieties and uncertainties these ambiguous findings can provoke. Edward’s insights ultimately encourage a balanced, personalized approach that elevates borderline ECGs from mere ambiguities to opportunities for proactive heart health management.
Building on Edward Philips’ detailed examination, this insightful commentary vividly captures the diagnostic uncertainty inherent in borderline ECG results. It highlights how such findings resist simple classification, reflecting subtle electrical variations influenced by diverse factors like electrolyte shifts, medications, or anatomical nuances. What stands out is the call to transcend reliance on the ECG tracing alone-underscoring the indispensable role of comprehensive clinical context, including symptom assessment and patient history, in shaping management decisions. Moreover, the emphasis on patient-provider communication is crucial; it ensures that uncertainties do not translate into undue anxiety or false reassurance but instead foster shared understanding and proactive care. In sum, the article thoughtfully positions borderline ECGs as a critical juncture inviting deeper exploration rather than premature conclusions, ultimately reinforcing patient-centered, nuanced cardiovascular evaluation.
Building on Edward Philips’ insightful analysis, this discussion aptly highlights the intricate balance clinicians must maintain when interpreting borderline ECGs. The “gray area” nature of these results underscores how the heart’s electrical activity cannot always be neatly categorized, necessitating a patient-centered approach that integrates clinical history, symptomatology, and risk factors. Importantly, Edward’s emphasis on the multifactorial causes-from electrolyte disturbances to anatomical nuances-reminds us that borderline findings are snapshots influenced by dynamic physiological variables. This compels careful follow-up rather than complacency. Furthermore, fostering transparent communication between provider and patient is essential to manage the inherent uncertainty-helping mitigate anxiety while ensuring vigilance. Ultimately, borderline ECGs are not diagnostic dead ends but invitations for comprehensive evaluation, reinforcing the nuanced nature of cardiovascular care and the need for personalized management strategies.