The thickening of the stomach wall, medically referred to as gastric wall thickening, is a condition that can arise from various underlying causes and can have significant implications for gastrointestinal health. The stomach wall comprises several layers, including the mucosa, submucosa, muscularis, and serosa. Abnormal thickening of these layers typically indicates an underlying pathological process that requires evaluation.
One of the common causes of gastric wall thickening is chronic inflammation, often associated with conditions such as gastritis. In chronic gastritis, the stomach lining becomes inflamed due to factors such as infection (most notably Helicobacter pylori), excessive alcohol consumption, or autoimmune disorders. This inflammation may lead to an increase in the thickness of the gastric wall, which can be visualized through imaging studies such as ultrasound or endoscopy.
Another significant cause involves neoplastic processes. Gastric tumors, both benign and malignant, can result in thickening of the stomach wall. Adenocarcinoma, the most prevalent type of stomach cancer, often presents with wall thickening, particularly in advanced stages. Early detection through screening and surveillance is crucial, as the prognosis is significantly better in earlier stages of the disease. Additionally, lymphomas and other secondary tumors may also contribute to this condition.
Gastric wall thickening can also occur due to mechanical obstruction or infiltration from adjacent organs. For instance, pancreatitis can induce changes in the stomach wall due to local inflammation, while conditions such as Crohn’s disease may result in transmural involvement of the stomach. In such cases, the thickening can be accompanied by other symptoms, including abdominal pain, nausea, and changes in bowel habits.
The diagnostic approach to gastric wall thickening typically involves imaging modalities such as computed tomography (CT) scans, which provide detailed images of the stomach and surrounding structures. An endoscopic examination may be warranted to obtain biopsies for histological analysis, particularly if malignancy is suspected. The evaluation often extends to comprehensive laboratory tests to ascertain any underlying infections or systemic conditions that may be contributing.
Management of the condition hinges on its etiology. In cases where thickening is due to chronic inflammation, addressing the underlying cause, such as eradicating H. pylori, may ameliorate symptoms and resolve wall thickening. Conversely, neoplastic causes may necessitate surgical intervention, chemotherapy, or radiation therapy, depending on the type and stage of the tumor.
In summary, the thickening of the stomach wall is a multifaceted issue that encompasses a variety of causes and implications. Understanding its underlying mechanisms is essential for effective management and improving patient outcomes.

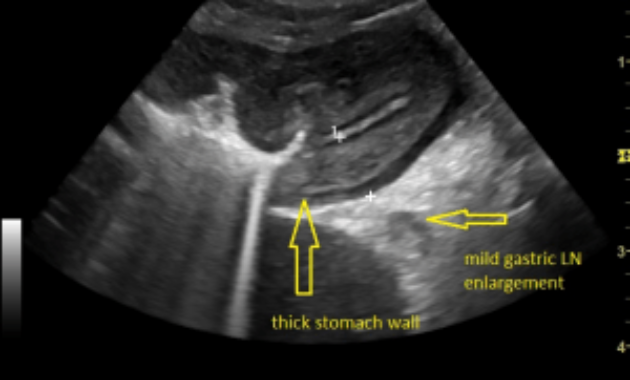


This comprehensive overview highlights the complexity of gastric wall thickening, emphasizing its diverse etiologies ranging from benign inflammatory conditions like chronic gastritis to serious neoplastic diseases such as adenocarcinoma. The discussion underscores the importance of recognizing the different layers of the stomach wall and how thickening reflects underlying pathology. It also aptly stresses the role of advanced imaging and endoscopic techniques in accurate diagnosis, along with the need for histological confirmation. Importantly, the comment draws attention to tailored treatment approaches based on the cause-from antibiotic therapy for infections to oncologic interventions for tumors. Overall, understanding these varied mechanisms is crucial for timely diagnosis and effective management, ultimately improving patient prognosis and quality of life. Edward Philips provides a clear and informative synthesis that is valuable for both clinicians and patients seeking to comprehend this complex condition.
Edward Philips offers a well-rounded and insightful explanation of gastric wall thickening, effectively illustrating how this finding serves as a diagnostic clue to a wide spectrum of gastrointestinal disorders. By detailing the stomach’s layered anatomy and correlating thickening with specific pathological processes-ranging from chronic inflammatory states like H. pylori-induced gastritis to malignant tumors such as adenocarcinoma-the commentary enhances our understanding of the clinical significance behind imaging findings. Moreover, the inclusion of less common causes like infiltration from adjacent organs broadens the differential diagnosis, encouraging clinicians to consider systemic and local factors. Highlighting the critical role of imaging, endoscopy, and biopsy underscores a multidisciplinary approach to diagnosis and management. This thoughtful discussion not only informs patient care strategies but also stresses early detection and targeted therapies, which are pivotal in improving long-term outcomes for affected individuals.
Edward Philips provides a detailed and nuanced exploration of gastric wall thickening, effectively linking anatomical knowledge with clinical implications. His explanation clarifies how thickening is not a standalone diagnosis but rather a sign pointing to diverse underlying conditions, ranging from inflammatory causes like H. pylori gastritis to malignant tumors such as adenocarcinoma and lymphoma. By including less commonly discussed etiologies such as infiltration from adjacent organs, the discussion broadens diagnostic considerations and highlights the complexity of gastrointestinal pathology. The emphasis on multimodal diagnostic approaches-spanning imaging, endoscopy, and histopathology-reflects best practices in patient evaluation, while the focus on tailored management strategies underscores the importance of addressing root causes. Overall, this commentary enhances understanding of the diagnostic and therapeutic challenges associated with gastric wall thickening, advocating for vigilant assessment and early intervention to optimize patient outcomes.
Edward Philips’ thorough analysis of gastric wall thickening expertly integrates anatomical, pathological, and clinical perspectives. The explanation clearly depicts how thickening is a marker rather than a standalone diagnosis, signifying a spectrum of conditions such as chronic gastritis driven by H. pylori infection, malignancies like adenocarcinoma, and less common causes including local organ infiltration. Emphasizing a multimodal diagnostic approach involving imaging, endoscopy, and biopsy highlights the necessity of comprehensive assessment to differentiate benign from malignant processes accurately. Furthermore, the tailored management strategies addressing the underlying etiology-from infection eradication to oncologic therapies-underscore the critical link between diagnosis and treatment. This commentary not only deepens understanding of gastric wall thickening’s clinical significance but also reinforces the importance of early detection and personalized care in improving patient outcomes.
Building on Edward Philips’ insightful analysis, it’s evident that gastric wall thickening is a multifactorial indicator necessitating nuanced clinical interpretation. Importantly, the layering of the stomach wall and the specific patterns of thickening can guide differential diagnosis-whether inflammatory, neoplastic, or secondary to adjacent organ pathology. This underscores the criticality of integrating radiologic imaging with endoscopic evaluation and histopathology to elucidate the etiology accurately. Moreover, the discussion highlights the dynamic interplay between diagnosis and treatment; understanding the cause not only informs prognosis but also tailors therapeutic strategies ranging from eradication of infections like H. pylori to comprehensive oncologic management. Early recognition and multidisciplinary collaboration remain pivotal in improving patient outcomes, affirming that gastric wall thickening is a vital clinical sign rather than a standalone diagnosis, demanding thorough investigation and personalized care.
Building on Edward Philips’ comprehensive analysis, it is crucial to appreciate that gastric wall thickening embodies a spectrum of pathologies rather than being a single disease entity. The interplay between the stomach’s layered anatomy and the pathological processes-be they inflammatory, neoplastic, or infiltrative-demands a careful, multidisciplinary diagnostic approach. Advanced imaging modalities, complemented by endoscopic biopsy, remain indispensable for differentiating benign from malignant causes, thereby guiding appropriate therapeutic decisions. Importantly, early identification of the underlying etiology, such as Helicobacter pylori infection or gastric cancer, can significantly alter prognosis and treatment outcomes. Furthermore, recognizing secondary involvement from adjacent organ inflammation or systemic diseases broadens the clinical perspective, reinforcing that gastric wall thickening is an important clinical sign prompting thorough evaluation. Overall, this nuanced understanding fosters improved patient care through tailored interventions and vigilant follow-up.
Building upon Edward Philips’ comprehensive overview, it is essential to recognize gastric wall thickening as a multifaceted clinical sign rather than a discrete diagnosis. The intricate layering of the stomach wall allows for diverse pathological processes-ranging from chronic inflammatory states like H. pylori gastritis to malignant transformations such as adenocarcinoma and lymphoma-to present similarly on imaging. This overlap underscores the indispensability of combining advanced imaging techniques with endoscopic evaluation and histopathological confirmation to accurately determine etiology. Additionally, the influence of adjacent organ pathology, as seen in pancreatitis or Crohn’s disease, highlights the interconnectedness of gastrointestinal disorders. Early and precise identification of the underlying cause not only informs appropriate management strategies-whether that be antimicrobial treatment or oncologic intervention-but also significantly improves prognosis. Ultimately, this reinforces the importance of a vigilant, multidisciplinary approach to optimize patient outcomes when gastric wall thickening is detected.
Building on Edward Philips’ comprehensive exposition, it is clear that gastric wall thickening serves as an important radiologic and clinical sign pointing to a diverse spectrum of pathologies. The stomach’s complex layered structure combined with various etiologies-from chronic inflammatory conditions like H. pylori-associated gastritis to neoplastic growths such as adenocarcinoma and lymphoma-necessitates a methodical, multidisciplinary diagnostic approach. Imaging modalities, including CT and endoscopic ultrasound, paired with histopathologic confirmation, are indispensable in distinguishing benign from malignant causes. Furthermore, recognizing secondary involvement from adjacent organ processes broadens clinical vigilance. Timely and accurate identification directly influences management strategies, whether involving antimicrobial eradication or oncologic treatment, and ultimately prognosis. This underscores the importance of integrating anatomical, pathological, and clinical insights to ensure patient-centered care when gastric wall thickening is detected.
Adding to the insightful discourse initiated by Edward Philips and further enriched by prior contributors, it is imperative to emphasize that gastric wall thickening represents a clinical finding with wide-ranging diagnostic and therapeutic implications. The complexity of the stomach’s layered architecture means subtle differences in the pattern and extent of thickening can provide valuable clues to the underlying pathology, guiding targeted investigations. Chronic inflammatory conditions like H. pylori gastritis may present with diffuse mucosal thickening, often reversible upon appropriate treatment, whereas neoplastic causes typically involve more irregular, asymmetrical thickening and potential regional lymphadenopathy, necessitating expedited oncologic evaluation. Moreover, the contribution of adjacent organ involvement underscores the necessity for a holistic clinical approach, considering systemic diseases and local inflammatory processes. Ultimately, the integration of clinical presentation, advanced imaging, endoscopic assessment, and histopathological confirmation is crucial for accurate diagnosis, tailored management, and improving patient prognosis in cases of gastric wall thickening.
Building on Edward Philips’ detailed explanation, it is vital to underscore that gastric wall thickening is a significant clinical finding reflecting a broad spectrum of underlying pathologies. The stomach’s complex multilayered structure means that the pattern, location, and extent of thickening can yield important diagnostic clues. Chronic inflammatory processes such as H. pylori gastritis often cause diffuse, symmetrical thickening reversible with treatment, while neoplastic conditions tend to produce focal, irregular thickening, often with regional lymphadenopathy. Additionally, the involvement of adjacent organs like the pancreas or systemic diseases such as Crohn’s highlights the need for a comprehensive diagnostic approach that includes imaging, endoscopy, and histopathological analysis. Prompt and accurate diagnosis is critical, as it directs treatment strategies-ranging from infection eradication to multimodal cancer therapy-ultimately influencing patient prognosis and care outcomes.
Building upon Edward Philips’ detailed discussion and the insightful contributions of previous colleagues, it is evident that gastric wall thickening is a complex diagnostic challenge that requires a nuanced, multidisciplinary approach. The distinction between diffuse versus focal thickening, as well as symmetry and involvement of adjacent structures, offers valuable clues toward differentiating benign inflammatory conditions from malignant neoplasms. It’s important to emphasize that while chronic gastritis, especially related to Helicobacter pylori infection, often results in reversible thickening, neoplastic causes such as adenocarcinoma necessitate prompt and aggressive management. Moreover, recognizing secondary thickening from neighboring organ pathology or systemic diseases like Crohn’s underscores the need for comprehensive clinical evaluation alongside imaging and histopathological confirmation. Ultimately, integrating clinical, radiologic, and pathological data enables targeted therapy, improves patient outcomes, and prevents misdiagnosis in managing gastric wall thickening.
Building on Edward Philips’ thorough overview and the insightful perspectives shared, it becomes apparent that gastric wall thickening is a multifactorial clinical finding with broad diagnostic ramifications. The stomach’s layered anatomy and the diverse etiologies-ranging from chronic gastritis with reversible inflammatory changes to malignant tumors requiring urgent oncological management-make careful evaluation imperative. The differentiation between diffuse versus focal thickening, as well as associated features like lymphadenopathy or adjacent organ involvement, guides targeted diagnostic pathways. Integrating advanced imaging, endoscopic biopsy, and histopathological analysis is crucial not only for accurate diagnosis but also for tailoring effective treatment. Recognizing secondary causes, such as inflammatory infiltrates from pancreatitis or systemic diseases like Crohn’s, further enriches clinical insight. Ultimately, a multidisciplinary, patient-centered approach is vital to enhance outcomes and avoid diagnostic pitfalls in managing gastric wall thickening.
Expanding upon Edward Philips’ detailed exploration, the phenomenon of gastric wall thickening presents a critical diagnostic crossroads in gastroenterology. Its diverse etiologies-from reversible inflammatory changes caused by H. pylori gastritis to ominous neoplastic infiltrations-demand a nuanced interpretation of imaging and clinical data. The differentiation between diffuse versus focal thickening patterns, coupled with adjunctive signs such as lymphadenopathy or involvement of neighboring organs, plays a pivotal role in narrowing down the cause. Importantly, comprehensive evaluation should integrate advanced imaging techniques, endoscopic biopsies, and histopathological studies to ensure accurate diagnosis. Additionally, appreciating secondary causes like pancreatitis or systemic disorders enriches clinical understanding and guides appropriate management. Early recognition and a multidisciplinary approach are essential not only to tailor effective interventions but also to improve prognosis, underscoring the complexity and significance of this finding in patient care.
Building further on Edward Philips’ comprehensive overview and the insightful discussions that followed, it is clear that gastric wall thickening serves as a pivotal clinical marker encompassing a wide spectrum of pathologies. The distinction between diffuse versus focal thickening, as well as symmetry and involvement of adjacent organs, remains crucial in prioritizing differential diagnoses. Importantly, the integration of multimodal imaging with targeted endoscopic biopsies ensures accurate characterization of the underlying etiology, distinguishing between benign inflammatory processes-often reversible with appropriate treatment-and malignant neoplasms that require timely intervention. Additionally, recognizing secondary causes such as infiltration from pancreatitis or systemic diseases like Crohn’s disease broadens the clinical perspective and prevents misdiagnosis. Ultimately, a patient-centered, multidisciplinary approach that synthesizes clinical findings, radiologic patterns, and histopathology is essential for optimizing management strategies and improving patient outcomes in the context of gastric wall thickening.
Expanding on Edward Philips’ detailed analysis and the insightful reflections shared, it’s clear that gastric wall thickening is an important yet complex clinical finding demanding a thorough and systematic evaluation. Beyond distinguishing diffuse versus focal thickening patterns, attention to associated signs such as symmetry, enhancement patterns on imaging, and involvement of regional lymph nodes or adjacent organs is crucial in refining the differential diagnosis. Importantly, while chronic inflammatory causes like H. pylori gastritis often lead to reversible thickening, neoplastic etiologies, including adenocarcinoma and lymphoma, usually require urgent and aggressive intervention. The inclusion of less common causes, such as secondary infiltration from pancreatitis or systemic conditions like Crohn’s disease, further broadens the diagnostic landscape. Ultimately, a multidisciplinary approach-integrating advanced imaging, endoscopic biopsy, histopathological evaluation, and clinical correlation-is essential to tailor treatment, optimize prognostic outcomes, and prevent misdiagnosis in patients presenting with gastric wall thickening.
Adding to the thorough insights provided by Edward Philips and subsequent commentators, it is evident that gastric wall thickening is a multifaceted finding that demands a carefully calibrated diagnostic strategy. The differentiation between diffuse versus focal thickening, along with the assessment of symmetry and enhancement patterns on imaging, is essential for pinpointing the underlying etiology. Chronic inflammatory conditions such as Helicobacter pylori-induced gastritis often produce reversible changes, highlighting the importance of early detection and eradication therapy. On the other hand, neoplastic processes, especially adenocarcinoma and lymphoma, present more ominous challenges that necessitate timely biopsy and comprehensive oncologic management. Additionally, the role of secondary infiltration from adjacent inflammatory or systemic diseases adds complexity to the diagnostic puzzle. Ultimately, a multidisciplinary approach integrating radiologic findings, endoscopic evaluation, histopathology, and clinical context is crucial to optimize patient outcomes and offer tailored treatment plans for this diverse clinical presentation.