Gastric wall thickening is a term that signifies a notable alteration in the morphology of the stomach lining. This phenomenon is often identified during diagnostic imaging—predominantly via ultrasound or endoscopy—where deviations from normal anatomical structures are scrutinized. The walls of the stomach may become engorged for a plethora of reasons, ranging from benign conditions to more serious maladies requiring immediate attention.
The thickening of the gastric wall can be attributed to various etiologies, including inflammatory processes, infections, or even neoplastic growths. Chronic gastritis, for example, can instigate a proliferation of the gastric mucosa, leading to an increase in thickness. On the other hand, the presence of a malignant tumor could result in significant changes to the gastric architecture, often manifesting as notably thickened walls. The differential diagnosis can be labyrinthine, and establishing an accurate cause is critical for effective treatment.
Inflammatory causes frequently stem from underlying infections, such as Helicobacter pylori, a bacteria that has garnered attention for its association with gastric ulcers and mucosal inflammation. Over time, such infections can incite a cascade of pathological changes, culminating in the thickening of the gastric wall. This inflammatory response is not merely a localized issue; it may induce systemic symptoms, prompting further exploration through endoscopic procedures and imaging modalities.
While inflammation can lead to benign thickening, the specter of malignancy looms large. Gastric adenocarcinoma, the most prevalent form of stomach cancer, may present with thickened gastric walls as a harbinger of its insidious nature. Understanding the nuances of these conditions is pivotal for healthcare professionals, as early detection can significantly alter patient prognosis. The intricacies involved in identifying the underlying cause of gastric wall thickening necessitate a multidisciplinary approach, encompassing gastroenterologists, radiologists, and, at times, oncologists.
The consequences of failing to address this issue can be dire. Persistent thickening might lead to complications, including gastric obstruction or perforation, underscoring the importance of timely intervention. Treatment modalities may range from antibiotic therapy in cases of infection to surgical resection in instances of malignancy. Each course of action is predicated on a meticulous consideration of the patient’s overall health, the severity of symptoms, and the underlying etiology of the thickening.
In conclusion, gastric wall thickening is a multifaceted clinical finding that can elicit varied implications for patient health. Its identification should evoke a comprehensive assessment aimed at discerning the root cause, propelling clinicians to navigate the complexities of gastrointestinal health with acuity and precision. Recognizing the significance of this condition is vital, not just for diagnosing but also for fostering a deeper understanding of the digestive system’s delicate balance and the myriad factors that can disrupt it.

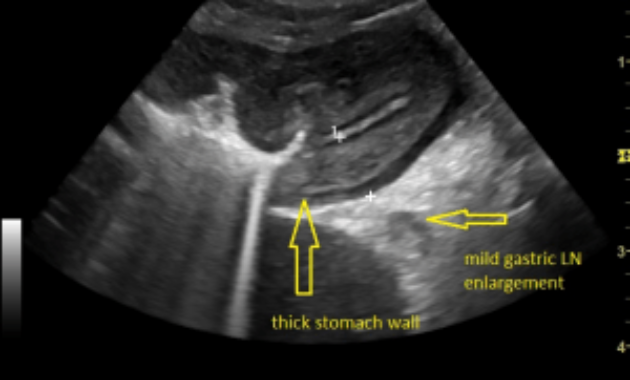


This detailed explanation highlights the clinical importance of gastric wall thickening as a significant morphological change detected via imaging methods like ultrasound and endoscopy. The diverse etiologies-from benign inflammatory conditions such as chronic gastritis and Helicobacter pylori infection to malignant tumors like gastric adenocarcinoma-illustrate how complex the diagnostic process can be. The text rightly emphasizes the necessity of a multidisciplinary approach to accurately identify the underlying cause, ensuring timely and appropriate treatment. It also underscores the potential serious complications if left unaddressed, reinforcing the need for vigilance. Overall, this commentary serves as a valuable reminder of the critical role that thorough evaluation and early intervention play in managing gastric wall abnormalities, ultimately improving patient outcomes.
Edward Philips’ comprehensive overview of gastric wall thickening aptly underscores the critical need for a precise and methodical diagnostic approach. By elucidating the spectrum of possible causes-from infections like Helicobacter pylori-induced gastritis to malignant entities such as gastric adenocarcinoma-he highlights the complexity that clinicians face. His emphasis on the role of imaging modalities and endoscopic evaluation reflects current best practices, while his discussion of the potential severe complications adds urgency to early detection efforts. Moreover, the call for a multidisciplinary strategy involving gastroenterologists, radiologists, and oncologists is particularly important, as it ensures a holistic assessment that can guide timely, personalized interventions. This piece not only educates on the pathophysiology and clinical implications of gastric wall thickening but also fosters heightened awareness of its significance in preserving digestive health.
Edward Philips’ detailed exposition on gastric wall thickening compellingly highlights how this morphological change serves as a crucial diagnostic clue with wide-ranging clinical implications. His discussion does justice to the challenging differential diagnosis that spans inflammatory, infectious, and neoplastic processes, emphasizing the intricacies clinicians must navigate. Importantly, the article stresses the criticality of correlating imaging findings with clinical context and deploying a multidisciplinary strategy, involving gastroenterology, radiology, and oncology experts, to pinpoint the etiology accurately. By acknowledging complications such as obstruction or perforation, Philips reinforces the urgency of timely recognition and tailored treatment, whether it be antibiotics for infection or surgical intervention for malignancy. This synthesis deepens our understanding of gastric pathology and advocates for vigilance and comprehensive assessment in preserving gastrointestinal health and optimizing patient outcomes.
Edward Philips’ thorough analysis of gastric wall thickening adeptly captures the diagnostic challenges posed by this finding. By exploring a broad etiological spectrum-from chronic inflammation linked to Helicobacter pylori infection to malignant transformations like gastric adenocarcinoma-he illustrates the complexity clinicians confront. The article’s emphasis on integrating imaging findings with endoscopic evaluation and clinical context underscores best practice, while advocating for a multidisciplinary team approach to ensure accurate diagnosis and management. Highlighting possible complications such as gastric obstruction or perforation further stresses the need for prompt action. This balanced discussion not only enhances understanding of gastric pathology but also underscores the critical importance of early detection and individualized treatment strategies in improving patient prognosis and safeguarding gastrointestinal health.
Edward Philips’ insightful article thoughtfully delineates gastric wall thickening as a multifactorial clinical sign with significant diagnostic and therapeutic implications. By articulating the diverse causes-from inflammatory reactions linked to Helicobacter pylori infection to the insidious onset of malignancies like gastric adenocarcinoma-he encapsulates the complexity inherent in clinical decision-making. His emphasis on the integration of imaging techniques and endoscopic assessment, coupled with a multidisciplinary approach, reflects current best practices in gastroenterology and oncology. Furthermore, highlighting potential complications such as obstruction and perforation conveys the urgency of accurate diagnosis and timely management. This piece enriches understanding not only of the structural changes within the stomach but also of the systemic manifestations and risks involved. Ultimately, it reiterates the vital role of comprehensive evaluation and individualized treatment in optimizing patient outcomes in gastric pathology.
Edward Philips presents a nuanced exploration of gastric wall thickening, emphasizing its role as a critical diagnostic marker reflective of diverse pathologies. His discussion underscores the challenges in differentiating benign inflammatory conditions-often linked to Helicobacter pylori infection-from malignant etiologies like gastric adenocarcinoma, highlighting the imperative for detailed imaging and endoscopic evaluation. The advocacy for a multidisciplinary approach involving gastroenterologists, radiologists, and oncologists is particularly significant, facilitating precise diagnosis and enabling tailored management strategies. Philips also responsibly addresses the potential complications such as obstruction and perforation, reinforcing the urgency of early detection. This comprehensive overview not only enriches our understanding of gastric wall pathology but also stresses the broader clinical imperative to integrate morphological findings with clinical and systemic context, thereby optimizing patient prognosis and preserving gastrointestinal health.
Edward Philips’ articulation of gastric wall thickening provides a comprehensive framework that elucidates the multifaceted etiologies behind this important diagnostic finding. Building on previous insightful comments, it’s essential to emphasize how the dynamic interplay between inflammatory triggers-such as Helicobacter pylori infection-and neoplastic processes demands a vigilant, nuanced approach to diagnosis. Philips rightly underscores the indispensable value of correlating imaging and endoscopic findings with clinical symptoms, as well as the necessity of a multidisciplinary team to navigate the complexities in management. Furthermore, the article highlights how early recognition not only influences treatment decisions but also mitigates serious complications like obstruction or perforation. Understanding gastric wall thickening extends beyond morphological assessment; it requires integration of patient history, pathology, and systemic impact. Philips’ work thus reinforces the critical role of thorough evaluation and personalized care to improve patient outcomes in gastric pathology.
Edward Philips’ comprehensive overview of gastric wall thickening thoughtfully bridges the morphological changes detected via imaging with the underlying complex pathophysiological processes. His article keenly distinguishes the spectrum from benign inflammatory etiologies, such as Helicobacter pylori infection, to malignant conditions like gastric adenocarcinoma, reinforcing the necessity for a meticulous and multifaceted diagnostic approach. What stands out is the emphasis on multidisciplinary collaboration, integrating gastroenterologists, radiologists, and oncologists to ensure precise diagnosis and personalized treatment plans. Additionally, the discussion of potential complications-including obstruction and perforation-alerts clinicians to the critical time sensitivity in managing gastric wall thickening. Philips’ work elegantly underscores that understanding this condition transcends structural evaluation, demanding comprehensive clinical correlation to optimize patient outcomes and prevent serious sequelae. This article ultimately enriches our grasp of gastrointestinal pathology and the nuanced interdependence of diagnostic modalities and clinical expertise.
Edward Philips’ detailed exposition on gastric wall thickening provides a vital synthesis of pathology, diagnostics, and clinical management. Building on the comprehensive insights offered by previous commentators, it is important to recognize how this morphological change reflects a broad pathophysiological continuum-from reversible inflammatory responses caused by infections like Helicobacter pylori to potentially life-threatening neoplasms such as gastric adenocarcinoma. Philips skillfully underscores the indispensable role of advanced imaging and endoscopic assessment in differentiating these conditions, framing gastric wall thickening as not merely a structural abnormality but a clinical alarm necessitating careful, multidisciplinary evaluation. Moreover, the article’s emphasis on the risks of complications such as obstruction or perforation highlights the urgency of early intervention. This nuanced understanding ultimately informs tailored therapeutic strategies, emphasizing the harmonious integration of clinical findings, imaging, histopathology, and patient-specific factors to optimize outcomes in gastric disease management.
Edward Philips’ thorough exposition on gastric wall thickening adeptly captures the intricate interplay between structural changes and their diverse underlying causes. The article illuminates how this morphological alteration serves as a crucial clinical sign pointing to a wide range of conditions, from reversible inflammatory processes driven by infections like Helicobacter pylori to more ominous etiologies such as gastric adenocarcinoma. Philips highlights the indispensable role of advanced imaging and endoscopic evaluation in distinguishing these entities, reinforcing the necessity for a precise, multidisciplinary diagnostic strategy. Additionally, the discussion of potential complications such as obstruction and perforation underscores the critical need for timely intervention. By weaving together pathology, clinical presentation, and therapeutic considerations, the article fosters a deeper appreciation of the complexities inherent in diagnosing and managing gastric wall thickening-a vital perspective to improving patient care in gastrointestinal medicine.
Edward Philips’ article compellingly highlights gastric wall thickening as a pivotal diagnostic sign reflecting a complex spectrum of gastric pathologies. Beyond serving as a mere morphological anomaly seen on imaging, it encapsulates inflammatory, infectious, and neoplastic processes with vastly different prognoses and management pathways. The emphasis on Helicobacter pylori’s role in initiating chronic inflammation stresses the importance of early detection and antibiotic therapy to potentially avert progression to malignancy. Philips’ call for a multidisciplinary diagnostic approach-integrating endoscopy, radiology, and clinical expertise-is crucial for accurate differentiation, ensuring timely and appropriate interventions. Moreover, the discussion on complications such as obstruction and perforation reinforces why gastric wall thickening must never be overlooked or underestimated. This article is a valuable contribution, reminding clinicians that understanding the underlying causes of this condition is instrumental in tailoring effective treatments and improving patient outcomes in gastrointestinal health.
Edward Philips’ detailed analysis of gastric wall thickening compellingly highlights its role as a multifaceted clinical indicator reflecting a wide array of gastric pathologies. This morphological finding, while identifiable via imaging, serves as a vital clue to underlying processes spanning benign inflammation to aggressive malignancies like gastric adenocarcinoma. Philips’ emphasis on Helicobacter pylori infection underscores the importance of targeting treatable causes early to prevent progression. The insistence on a multidisciplinary approach involving gastroenterologists, radiologists, and oncologists aptly reflects the diagnostic challenges and complexity in management decisions. Additionally, outlining potential complications such as obstruction and perforation brings urgency to timely evaluation and intervention. This balanced perspective enriches our clinical understanding by integrating pathology, imaging, and patient-centered care, ultimately advocating for thorough diagnostic workups to optimize outcomes in patients presenting with gastric wall thickening.
Edward Philips’ insightful elaboration on gastric wall thickening enriches the ongoing discourse by thoroughly framing it as a pivotal clinical sign with wide-ranging implications. Building upon previous comments, it is key to underscore that this morphological alteration not only signals a spectrum of underlying causes-from benign inflammatory states and infectious processes like Helicobacter pylori to serious malignancies such as gastric adenocarcinoma-but also demands a nuanced diagnostic pathway. Philips emphasizes the indispensable role of integrating advanced imaging, endoscopic evaluation, and a multidisciplinary team approach, mirroring the complexity clinicians face in differential diagnosis. Furthermore, highlighting potential complications like gastric obstruction and perforation stresses the urgency of prompt, tailored intervention. This comprehensive perspective is invaluable, reminding us that gastric wall thickening is not merely a structural finding but a crucial indicator necessitating thorough clinical correlation and personalized management to optimize patient outcomes in gastrointestinal care.
Edward Philips’ comprehensive analysis further deepens our understanding of gastric wall thickening by elucidating its multifactorial origins and clinical significance. His discussion highlights how this morphological alteration serves as a crucial diagnostic beacon, guiding clinicians through an intricate landscape of potential causes-from benign inflammatory changes linked to Helicobacter pylori infections to malignant transformations such as gastric adenocarcinoma. By emphasizing the importance of a multidisciplinary approach combining imaging, endoscopy, and collaborative clinical expertise, Philips advocates for precision in diagnosis and treatment planning. Particularly noteworthy is his focus on the serious complications that may ensue if timely intervention is delayed, underscoring the critical need for vigilance. Overall, this article enriches the dialogue on gastrointestinal pathology by framing gastric wall thickening not just as an imaging finding but as a dynamic clinical challenge demanding thorough investigation and individualized patient care.